Dynamic Hyperinflation and Auto-PEEP
Pathogenesis
No concept is more important in understanding and managing mechanical ventilation in patients who have obstructive lung disease than that of dynamic hyperinflation. As mentioned above, COPD and asthma are characterized physiologically by hyperinflation and expiratory airflow limitation. When airway obstruction is severe, sufficient time may not be available to exhale completely a given tidal breath prior to the next inspiration. This means that that next breath begins at a higher lung volume. Over the course of several such breaths, the patient becomes progressively hyperinflated, and reaches a new FRC considerably higher than that at which the sequence began. Patients who have severe COPD may experience this phenomenon spontaneously during panic attacks or at times of increased dyspnea, but it can be especially serious during positive-pressure ventilation.
Clinical manifestations
As a result of the elastic recoil of the lung when distended above FRC (and of the chest wall at even larger lung volumes), dynamic hyperinflation is associated with positive end-expiratory alveolar pressure, or auto-PEEP (also called intrinsic PEEP, dynamic PEEP, or endogenous PEEP). The physiologic effects of auto-PEEP are the same as those of dialed-in (extrinsic) PEEP, and include decreased cardiac preload because of diminished venous return into the chest. The reduced cardiac output that results from the reduction in preload can lead to hypotension and, if severe, to pulseless electrical activity and cardiac arrest. Dynamic hyperinflation can also lead to local alveolar overdistention and rupture, followed by pneumothorax and other forms of extra-alveolar air (clinical barotrauma, see below).
Auto-PEEP is common in ventilated patients who have underlying COPD. Several other clinical circumstances suggest an increased likelihood of dynamic hyperinflation and auto-PEEP. Of special importance is the circumstance in which the patient appears to exert unusual effort to trigger the ventilator, or if airflow from the ventilator is not initiated with every inspiratory effort. Figure 7 illustrates why the latter occurs.
Fig 7
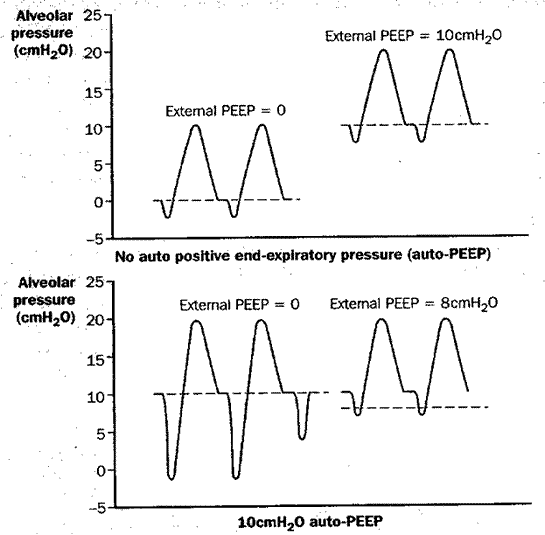
Figure 7: Impact of dynamic hyperinflation and auto-PEEP on a patient’s ability to trigger the ventilator, and the effect of adding external PEEP. Upper diagram: Triggering the ventilator in the absence of auto-PEEP. The addition of external PEEP does not affect the relative ease of initiating breaths from the ventilator. Lower diagram: Triggering the ventilator in the presence of 10 cm H2O of auto-PEEP. In the absence of external PEEP (left portion of each figure), in order to initiate inspiratory flow from the ventilator, the patient must generate enough ventilatory muscle contraction to overcome the 10 cm H2O of auto-PEEP in order to reduce tracheal pressure below zero. One occasion (lower left, 3rd breath attempt), insufficient force is generated to trigger the ventilator. When 8 cm H2O of external PEEP is added, the patient can trigger the ventilator much more easily, since much less ventilatory muscle contraction is needed to bring tracheal pressure down to the external PEEP level in order to initiate inspiratory flow.
Detection and measurement
Unlike externally applied PEEP, which is indicated on the ventilator’s pressure manometer, auto-PEEP cannot be detected unless a special maneuver is performed to allow pressures to equilibrate from the patient’s alveoli to the exhalation valve of the ventilator circuit at end expiration. At the author’s institution, respiratory practitioners who care for ventilated patients routinely check for the presence and magnitude of auto-PEEP (at least once each shift) in every patient who does not make spontaneous ventilatory efforts. When patients breathe spontaneously or attempt to trigger the ventilator, the end-expiratory occlusion technique cannot be used, and a different method such as stepwise addition of external PEEP must be used. Table 12 [21k PDF*] lists the different techniques available for detecting and quantitating auto-PEEP.
Prevention and management
The key to prevent the development of dynamic hyperinflation, and to reduce its severity when present, is to increase expiratory time. Dynamic hyperinflation occurs because insufficient time is available to complete lung emptying following each positive-pressure breath. Therefore, prevention and management hinge on measures to reduce airway obstruction, and to decrease the time spent on inspiration during each minute. Table 13 [15k PDF*] lists practical steps that can be taken to prevent auto-PEEP in ventilated patients, and to minimize it when present.
If the patient makes active inspiratory efforts, the addition of external PEEP decreases the muscular effort needed to trigger breaths from the ventilator, and thus decreases work of breathing and increases patient comfort. The added external PEEP should be at about 80% of the measured or estimated auto-PEEP level, as the latter is an average of various actual auto-PEEP levels in different lung regions, some of which are lower than the measured auto-PEEP. The level of auto-PEEP is checked frequently as the patient’s condition changes, with adjustments in external PEEP made accordingly.
 Top of Page
Top of Page
< Previous:
Complications Associated With Invasive Mechanical Ventilation
| Next: Barotrauma